PsA Causes: What are the Main Causes of Psoriatic Arthritis?
Do you suffer from psoriasis? Do you also experience joint pain and inflammation? Have you been tested for psoriatic arthritis?
Psoriatic arthritis (PsA) is one of the three most common types of arthritis, along with rheumatoid arthritis. Men and women are equally affected by the disease. About 1-2 people per 1000 in the general population suffer from PsA. According to the National Psoriasis Foundation, the onset of PsA usually occurs in your fourth and fifth decade. Eighty-five percent of individuals with PsA also have psoriasis.
On the flip side, up to thirty percent of the individuals with psoriasis (characterized by red, itchy patches of skin, usually covered in silver scales) will develop PsA. Of patients with psoriasis who did not have PsA at presentation, almost 2 percent per year will be diagnosed with PsA.
What are the Symptoms of Psoriatic Arthritis?
What are some of the signs of PsA? There are five patterns of joint manifestations of PsA. These are based on how (and which) joints are affected. Most of the actual symptoms that you experience are the same for all of the patterns of the disease. The five patterns of PsA are:
- Symmetric polyarthritis – characterized by joint inflammation occurring on both sides of the body equally (presents similar to rheumatoid arthritis)
- Asymmetric oligoarthritis – characterized by joint pain that involves less than 5 different joints on both sides of the body
- Spondyloarthritis – characterized by pain and inflammation affecting the spine
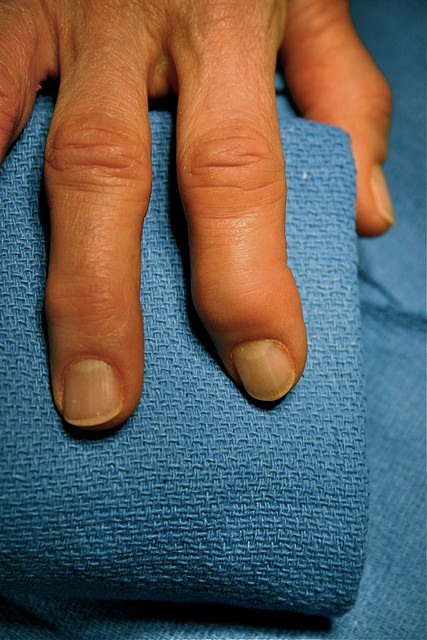
- Distal arthritis – characterized by joint pain and inflammation affecting the distal joints of the fingers and toes (specifically the DIP joints)
- Arthritis mutilans – the most severe form, which often causes deformities in the hands and feet
Some patients will present with more than one pattern, and their pattern of disease may change through the course of their lifetime. Because these patterns can change over time, PsA manifestations are simplified into 5 clinical areas:
- Peripheral arthritis – inflammation of extremities
- Axial disease – inflammation of the spine
- Enthesitis – inflammation at tendons, ligaments, synovium
- Dactylitis – diffuse swelling of entire finger or toe
- Skin and nail disease
The following are some of the more common symptoms of PsA. You don’t have to experience all of the symptoms to be diagnosed with PsA. However, if you suspect you might be suffering from PsA, you should see a doctor to confirm the diagnosis. Symptoms can include:
- Joint pain
- Joint swelling
- Swelling of the fingers and toes – “sausage digits”
- Back pain (can indicate psoriatic spondylitis)
- Foot pain
- Joint stiffness (especially when waking or after resting for a period of time)
- Tendon or ligament pain
- Nail pitting and/or infected looking nail beds
- Fatigue
- Reduced mobility
- Eye pain
What Causes Psoriatic Arthritis?
PsA is a chronic autoimmune disorder where the body is essentially attacking itself. That is, your body’s immune system starts attacking healthy cells and tissue. This autoimmune response is the cause of the joint pain and inflammation.
But what causes the PsA? Unfortunately, little is known about the true cause of PsA; however, it is believed that both genetics and the environment are at play. You are at an increased risk of developing PsA if your family members have psoriasis or PsA. Environmentally speaking, some believe having certain viral or bacterial infections can increase your chances of developing PsA.

The three largest risk factor for developing PsA include:
- Having psoriasis – this is the leading cause of developing PsA
- Your family history – there is a genetic link with this disease – many individuals who have PsA also have a sibling or parent with the disease
- Your age – While you can develop PsA at any age, the disease’s onset is most likely to develop between the ages of 40 and 50
While the true cause of PsA is unknown, there has been a link among individuals who have psoriatic spondylitis (psoriatic arthritis of the spine) and a specific gene marker. In 50% of individuals who suffer from PsA of the spine, HLA-B27 is present.
Stressful life events can also cause PsA to flare for the first time in individuals predisposed to the disease or in individuals who have already been diagnosed with the disease.
Additionally, the onset of PsA has been linked to individuals who experienced strep throat, pointing to possible viral and bacterial links to at least the onset of the disease.
Obesity can also increase an individual’s risk of developing PsA.
What Causes Flare-ups?
If you’ve already been diagnosed with PsA, you will notice that your symptoms tend to wax and wane. These periods of increased severity of symptoms are called “flares” or “flare-ups” and are very common in individuals who have the disease. While several things may cause flare-ups, the following are the most common:
- Stress – try to reduce stress as much as possible
- Skin trauma – including cuts and scrapes. This is known as the Koebner phenomenon
- Dry skin – keep skin moisturized
- Sunburn – getting sun helps psoriasis; however, sunburns exacerbate the situation
- Certain medications – antimalarial drugs, beta blockers, and lithium have all been known to increase psoriatic arthritis flare-ups
- Climate – any type of climate that can cause dry skin can increase your risk for flare-ups
- Alcohol consumption – alcohol can interfere with the uptake of medications and also increases your risk of flare-ups
- Gluten – gluten, found in certain grains (barley, wheat, and rye) can cause flare-ups
- Common infections – Upper respiratory infections, including thrush and strep throat
How is Psoriatic Arthritis Treated?
PsA can be treated through medications and lifestyle changes. Medications most often prescribed include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Immunosuppressants
- Tumor necrosis factor-alpha (TNF-alpha) blockers
- Disease modifying anti-rheumatic drugs (DMARDs)
- Steroids
Medications can only treat the symptoms of PsA. However, lifestyle changes can help to reduce flare-ups and increase mobility. Some lifestyle changes include:
- Exercise
- Stress-reduction techniques
- Eating a healthy diet
When you experience repeated PsA flare-ups, you might be able to notice a trend in certain triggers (e.g., stress, eating a certain type of food). If you can spot these triggers, you can concentrate on trying to eliminate or reduce them from your environment.
Psoriatic Arthritis Prognosis and Outlook
What is the prognosis for individuals who experience PsA? Some of it depends on the pattern of PsA you have. But, overall, the sooner you are diagnosed and begin treatment, the better your prognosis and pain will be.

While PsA is a chronic, yet progressive disease, in that it tends to get worse over time, you may have a milder form that doesn’t cause too much pain and decreased mobility. For example, the most common type of PsA, asymmetric oligoarticular, tends to come with the mildest symptoms. In contrast, the rarest form, yet the most debilitating form, arthritis mutilans, can cause severe deformities.
Whatever the type of PsA you have, the sooner you receive treatment and the more vigilant you are in making lifestyle changes, the less pain and better quality of life you will experience.
