Remicade: How Effective is Remicade in Treating RA?
When you suffer from Rheumatoid Arthritis, you suffer from swollen, painful joints throughout your body. In more severe cases, long-term exposure to joint inflammation can cause bone erosion and joint deformity and the loss of mobility.
There is no cure as yet for Rheumatoid Arthritis, but there are methods to manage its painful symptoms and slow down or halt the progression of the disease altogether. Medications, homeopathic remedies, and physical therapy have all been shown to be helpful in the treatment of RA. One medication, in particular, has been found to have a significant impact on the treatment of Rheumatoid Arthritis, especially in moderate to severe cases of the disease. This drug is called Remicade.
What is Remicade?
Remicade is a drug treatment method for Rheumatoid Arthritis that is given intravenously. It’s usually prescribed for patients who are experiencing aggressive RA symptoms in an effort to halt the progression of symptoms and joint damage.
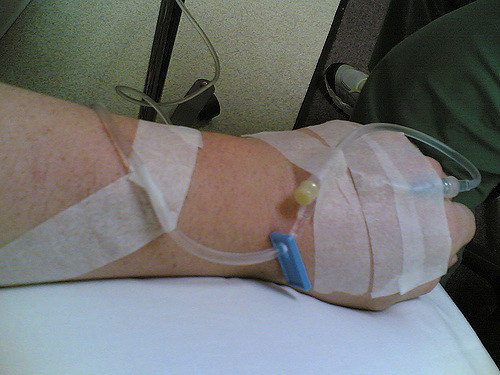
Known generically as Infliximab, Remicade is a monoclonal antibody that is used in RF to disrupt the occurrence of joint inflammation. Specifically, it binds to TNF-a, a chemical messenger crucial to the inflammatory process, preventing it from stimulating inflammation, and thus helping to prevent joint pain and damage. Remicade works to block the signal for the stimulation of more inflammation and progression of the disease.
How to Take It
As stated above, Remicade is given intravenously. And, often in combination with methotrexate, another common medication for the treatment of RA. Remicade is usually prescribed in combination with methotrexate to enhance the effectiveness of both drugs.
As Remicade is given intravenously, you’ll need to visit a doctor’s office or an outpatient treatment center to receive the drug. As a dose of Remicade is not a simple shot or injection, it’s an actual transfusion. Administration of the drug takes approximately two hours. Remicade comes in powdered form, which is then mixed with water for infusion. The mixture is placed in a transfusion bag and dripped slowly intravenously. During administration, your blood pressure will be checked periodically and a nurse will assess you for the side effects of the drug.
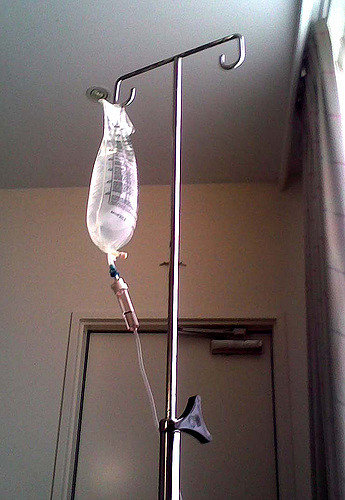
The dosage of Remicade is based on a patient’s weight. The recommended dose is 3 mg/kg. Heavier patients will need more Remicade than lighter patients. After the initial dose of 3mg/kg, additional doses of 3mg/kg should be given at two and six-week intervals. Maintenance doses of Remicade are administered at eight-week intervals.
It’s important to note that a single dose of Remicade is very expensive and is sometimes not covered by insurance. A single dose typically ranges from $1,300 to $2,500. Medicare does not cover Remicade. Prior to beginning Remicade, you should work with your doctor’s office to determine insurance options. Remicade can be covered by insurance, though the doctor’s office will likely have to answer a number of questions for the insurance company (why other treatments didn’t work, why Remicade is being recommended, etc.).
Side Effects
In general, the side effects of Remicade have been pretty mild. The most common side effects of the drug are rashes and headaches. However, other side effects that have been reported include:
- Nausea
- Vomiting
- Back pain
- Urinary tract infections
- Abdominal pain
- Fever
Right after the IV infusion is completed, some patients experience changes in blood pressure, difficulty breathing, chest pain, itching, fever, and chills. Let your doctor or nurse know if you are experiencing any of these symptoms, as they might indicate an allergic reaction to the drug.
Warnings and Precautions
Because of drug interactions, there are a number of conditions you should tell your doctor about prior to taking Remicade.

If you have any of the following, please consult with your doctor:
- Congestive heart failure
- Multiple Sclerosis or other nervous system disorders
- Lupus
- Cytopenia
- Tuberculosis
- Diabetes
- Immune system disorders
- Cancer
- Hepatitis B
- Liver disorders
- Psoriasis
While there have been no significant studies of the effects of Remicade in pregnancy, Remicade should only be used while pregnant if absolutely necessary. Remicade is transferred to the baby via breast milk, so you should not breastfeed while using Remicade.
