PsA Facts: How Prevalent is Psoriatic Arthritis?
You’ve heard of arthritis. You’ve heard of psoriasis. But, have you ever heard of psoriatic arthritis? Sharing a number of symptoms and treatments with other types of arthritis and arthritic-type conditions (e.g., rheumatoid arthritis, osteoarthritis, and gout), psoriatic arthritis has one major distinguishing characteristic: those that live with this disease either have a personal or family history of psoriasis.
In fact, a medical history of psoriasis should be an alert that any pain or swelling in the hands or feet may be symptoms of psoriatic arthritis. Patients diagnosed with psoriasis should be on the alert for signs and symptoms of arthritis.
Psoriatic Arthritis By the Numbers
Psoriatic arthritis question and answer:
How many people have psoriatic arthritis? In the United States psoriasis occurs in about 2% of the population and equally among the sexes. In people diagnosed with psoriasis, about 5%to10% will go on to develop psoriatic arthritis.
When do individuals first begin noticing symptoms? Around 85% of individuals living with psoriatic arthritis have lived with psoriasis for years prior to the onset of arthritis. Symptoms of psoriatic arthritis typically occur between ages 30 and 50, with most cases starting between the fourth and fifth decade.
Does everyone with psoriasis get psoriatic arthritis? No. Studies have shown that anywhere from 5% to 30% of individuals living with psoriasis will go on to develop psoriatic arthritis. This wide discrepancy in incidence is due to variations in definitions and design from one clinical trial to another over time.
Are there different types of psoriatic arthritis? There are five types of psoriatic arthritis: symmetric (affecting the same joints on both sides of the body), asymmetric (affecting joints on one side of the body), distal interphalangeal (affecting joints in the fingers and toes), spondylitis (affecting the spine and lower back), and arthritis mutilans (causing severe deformity in the fingers and toes).

How many people are severely affected by psoriatic arthritis? About 20% of individuals living with psoriatic arthritis are characterized as suffering from severe psoriatic arthritis – affecting four or more joints.
Is psoriatic arthritis curable? Unfortunately, no, not yet. Psoriatic arthritis is a chronic and progressive disease, with 55% of individuals living with the disease developing five or more deformed joints after 10 years.
How can doctors tell if you have psoriatic arthritis? Doctors will conduct a history and physical exam and also conduct blood-work to look for the presence of psoriatic arthritis-specific antigens and also to rule out antigens present in the bloodstream with other types of arthritis.
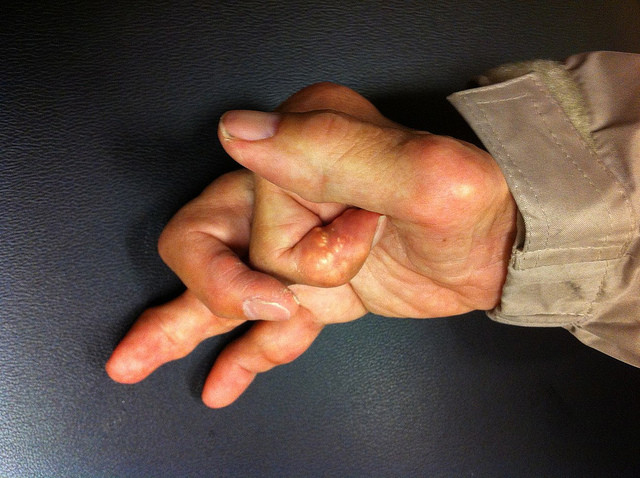
What are the most common symptoms of psoriatic arthritis? The presence of psoriasis occurs in approximately 85% of individuals living with psoriatic arthritis. Also prevalent is nail pitting and nail changes that are present in 87% of individuals living with psoriatic arthritis. Dactylitis, which causes the fingers and toes to swell up so much they have a “sausage-like” appearance occurs in about 50% of individuals with psoriatic arthritis.

Does psoriatic arthritis only affect the joints? Psoriatic arthritis affects the tendons and the ligaments in about 50% of patients who suffer from the disease. Additionally, psoriatic arthritis can have systemic manifestations including involvement of the eyes and other organs.
Can psoriatic arthritis occur in children? While the overwhelming majority of cases of psoriatic arthritis occur in adults, children can be diagnosed with psoriatic arthritis. The typical age of onset of juvenile psoriatic arthritis is between 9 and 11 years of age.
Psoriatic Arthritis Key Facts
Psoriatic arthritis is an chronic autoimmune disease
An autoimmune disease is present when your body’s immune system is mistakenly stimulated to attack your own normal organs and tissues. With psoriatic arthritis, your body is attacking healthy joint tissue, causing inflammation, pain and swelling. As of yet there no cure for psoriatic arthritis.
Symptoms wax and wane with psoriatic arthritis
Known as “flares,” psoriatic arthritis symptoms come and go. You could have no symptoms of psoriatic arthritis for days or months and all of a sudden, they appear again. Complete with pain, swelling, inflammation, tendonitis, and related problems. In rare cases, individuals with psoriatic arthritis seem to go into a remission state, exhibiting no symptoms for years. However, many years later, symptoms tend to return.

Distinguishing characteristics
Having joint pain on only one side of the body? Does swelling occur down the full-length of your fingers and toes (instead of just concentrated in the first or second joints)? Has your blood-work tested negative for Rheumatoid Factor (RF)? Do you have psoriasis (or have you suffered from psoriasis in the past)? Then all signs are pointing toward a diagnosis of psoriatic arthritis.
It looks a lot like Rheumatoid Arthritis
At first glance, psoriatic arthritis looks a lot like rheumatoid arthritis. In fact, it’s the subtle differences between the two diseases that are key to a proper diagnosis. Rheumatoid arthritis typically affects both sides of the body symmetrically. And, you’ll test positive for Rheumatoid Factor (RF) when your doctor conducts a blood-test. Even trickier, psoriatic arthritis also looks a lot like osteoarthritis and gout. Only your doctor will be able to make a confirmed diagnosis.
Gender Characteristics
Psoriatic arthritis is pretty gender neutral – affecting men and women equally. Whereas rheumatoid arthritis tends to affect woman three times more than men.
It is likely hereditary
The true cause of psoriatic arthritis is unknown. However, most scientists believe genetics plays a important role. In fact, 40% of individuals who have psoriatic arthritis also have a relative who has psoriatic arthritis or a relative with psoriasis. That’s a greater genetic link than any other type of rheumatic disease.
You can’t “catch” psoriatic arthritis
Psoriatic arthritis is not contagious. Nor is psoriasis. However, environmental triggers of the disease can be contagious. Certain viral and bacterial infections, such as strep throat, which are highly contagious, and cause physiologic stress are thought to “jump-start” the onset of psoriatic arthritis. The reason behind this type of connection is that it activates an already out of whack immune system.
It affects more than the joints
When most people think of arthritis, their thoughts center around joint pain and inflammation. Psoriatic arthritis definitely affects the joints. But, it also can cause a host of other secondary conditions. Some of the most common secondary conditions include tendonitis, eye problems (like conjunctivitis and uveitis), associated metabolic syndrome (affecting your blood pressure and cholesterol levels) leading to a higher risk of diabetes and heart disease.
You may not look sick
Your symptoms might not be flaring up. You might not have skin lesions and noticeable psoriasis. Your fingers and toes might not look like sausages. But, that doesn’t mean you aren’t still in pain and still suffering from intense fatigue. Sometimes, friends and family might not understand how much pain you are in because they don’t physically see the symptoms.
Treatment options are available and helpful
The good news? Over-the-counter (OTC) and prescription medications are available and have great success rates for individuals living with psoriatic arthritis. NSAIDs and DMARDs are two of the most effective types of medications in treating psoriatic arthritis. Additionally, lifestyle changes can help to manage the symptoms and contribute greatly to a state of well-being for individuals living with psoriatic arthritis. Participating in joint-gentle exercise routines, incorporating regular rest periods into your daily routine, and controlling your weight to keep stress off of your joints are all proven methods of helping ease the pain associated with psoriatic arthritis.
